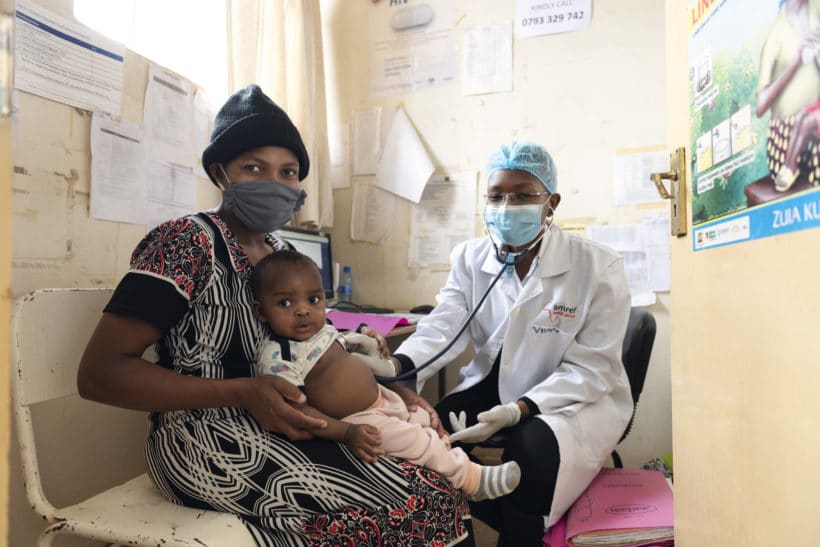
Deliveries of COVID jabs to Africa have been ramped up in recent months, but the poor provision of health services in rural areas threatens to undermine vaccination efforts.
While we urge rich countries to quicken the pace of vaccine distribution to Africa – which remains unpredictable and erratic – there must be simultaneous efforts to ensure that hundreds of millions of Africans living in villages and other remote areas are not overlooked as rollouts gain momentum.
Failure to do so will continue to leave countries in the region vulnerable to the virus and new variants, even if donors substantially boost deliveries of jabs to the continent.
Already, there are alarming signs of vaccine distribution inequalities within countries. In Kenya for example, 40-50% of people in urban areas are vaccinated, compared to less than 10% in rural parts of the country, according to health ministry data.
46% of Kenyan doctors are located in or around Nairobi, home to less than a fifth of the national population. It’s the same picture in Angola and South Africa. The rural shortages are exacerbated by health worker migration. Doctors choose to practice in Europe, the US, Asia and the Middle East, where they are better paid: 63% of newly-trained doctors in Africa end up practicing abroad.
The root of the geographic inequalities is the chronic underfunding of Africa’s healthcare systems. While the US spends $10,000 per capita on health, the corresponding figure in Africa is just $70.
We have fewer healthcare workers per population than anywhere else in the world. There are, on average, three physicians per 10,000 population, compared to ten times that number in OECD countries.
Too often in rural areas women end up giving birth without skilled medical assistance while children with pneumonia or malaria struggle to get treatment because the nearest hospital is too far away.
Logistical difficulties are also limiting COVID vaccination rollouts. And the problem is compounded by donor deliveries of consignments of vaccines with short expiry dates. Overstretched urban healthcare workers struggle to use them in time, never mind their more remote counterparts.
Clearly, as a priority, Africa needs more vaccines and certainly ones with longer shelf lives. But no less important, a large increase in the number of healthcare workers, especially in rural areas, is needed. The COVID19 Africa Commission, chaired by President Ramaphosa, is creating an Africa Health Workforce Task Team to evaluate the health workforce needs of the continent and set targets on how to bolster their ranks.
It’s a commendable initiative. But we are running out of time. Right now, we need urgent interventions to ensure more equitable distribution of COVID jabs, or risk seeing all the good vaccination work in towns and cities unravel as they succumb to new outbreaks originating in largely unvaccinated rural areas.
Encouragingly, there have been some innovative solutions driven by governments and civil society organisations.
In the US and much of Europe, pharmacists did most of the heavy lifting in vaccinating the population. In many African countries, only doctors and nurses are legally permitted to administer jabs, but Zimbabwe trained pharmacists to offer vaccinations.
At the same time, Amref has flown thousands of vaccines out of Nairobi to remote and insecure parts of Kenya. We also run outreach at health facilities on weekends for the vast majority of people too busy making a living the rest of week when routine vaccinations, including COVID vaccination, are offered.
In one Saturday, outreach in Kibera, the informal settlement in Nairobi, our team jabbed 350 people in six hours at a health centre that vaccinates a handful of people on a weekday. Taking vaccines to the people while paying attention to their lives makes good sense.
Ultimately, Africa needs to spend much more per capita on healthcare to begin to really address the urban-rural medical provision divide. We hope the Africa Health Workforce Task Team will provide valuable data on continent-wide needs.
Countries can also fill the urban rural gap by employing community-based health officers who would complement essential appropriate primary care services at the village level. There should be an expansion of mobile phone–based “telemedicine” and diagnostics that connect health workforce and rural communities.
In Rwanda and Ethiopia, community health workers from villages were trained to give primary care and refer people to higher health facilitiesfor serious illness. (source). By 2016, there were 45,000 of these community health workers in Rwanda and 35,000 in Ethiopia.
At Amref, we have innovated mobile vans, which can be equipped with coolers to transport refrigerated vaccines, medicines and lab samples to and from faraway health clinics.
But, in the meantime, the international community must support and encourage local government and NGO initiatives to address current vaccine distribution inequalities. Individual interventions may be limited in scope but together they could significantly improve vaccination rates in rural areas.
Dr. Githinji Gitahi is Group CEO of Amref Health Africa. Charles Okeahalam is Chairman of Amref Health Africa’s international board of directors